Welcome to this article from Optometry-Evolution on how we can best help our visually impaired patients in Optometry practice.
 In my last hospital optometry role I did regular low vision clinics for about 12years. The vast majority of the patients seen were elderly and had some degree of visual loss due to AMD. In this time, I tried to develop an approach that considered the needs, and often the worries of the patient and how I could best help. There is such variation in the level of visual impairment, the demands of the patients, their motivation, their general health and everyday quality of life, that we cannot apply a ‘one size fits all’ approach.
In my last hospital optometry role I did regular low vision clinics for about 12years. The vast majority of the patients seen were elderly and had some degree of visual loss due to AMD. In this time, I tried to develop an approach that considered the needs, and often the worries of the patient and how I could best help. There is such variation in the level of visual impairment, the demands of the patients, their motivation, their general health and everyday quality of life, that we cannot apply a ‘one size fits all’ approach.
The aim of this article is to give an overview of the measures community optometrists can take to help their patients who have some degree of visual impairment and help make improvements to their quality of life.
Visual impairment can often lead to frustration for the patient, reduce their independence and leave them feeling isolated. As optometrists we are well placed to play our part in helping to prevent this from being the case.
The scope of this article is really intended to cover those patients with mild to moderate visual loss. Those who have significant loss or more complex needs should be referred for specialist low visual aid support.
Chat to the patient
As with every patient consultation, having a good overview of their symptoms and difficulties in relation to their visual performance and condition is key. Listen to the type of tasks and situations that are causing the patient problems. Often this is reading and other near tasks due to central visual loss due to AMD, or it could be reduced navigational vision due to advanced glaucoma.

Have an understanding of their life-situation; do they live alone, do they have relatives/support nearby, still drive, are they employed, do they study or care for a relative? Also have an appreciation of other health problems they have which might be getting compounded by their visual impairment – they might have reduced mobility, reduced dexterity, difficulties accessing treatment for other conditions or cognitive difficulties for example.
So building a picture as to the type of difficulties they are having can help you target your management as best possible.
Reading
The following strategies may help with reading function:
- Optimise the reading spectacles. For patients with mild impairment, an increased near addition, used with a shorter than normal working distance can help with print. The advantage here is that it may avoid the use of a magnifier, and be a more ‘normal’ sense of reading for the patient. The patient needs to be well counselled on the short working distance. Often considering a near-add in the range of +4.00 to +6.00, with possible base in prism to aid convergence, if you go beyond +6.00.
- Magnifying glasses. There is a whole range of devices that can be considered. This usually depends on the level of vision, the task involved and the ability of the patient to hold the lens.

- The usual starting point is to consider a hand-held magnifier. A lens that is illuminated with an LED light is ideal in order to improve the contrast of the text the patient is trying to read. Something like a X3.5 or X5 LED hand held magnifier can be a good starting point for a lot of patients. Once you go beyond this strength, the field of view can become restricted.
- Using a small non-illuminated pocket magnifier can be really useful for the patient to have in their pocket for when they are out and about and just wanting to spot short pieces of information such as prices and labels in shops.
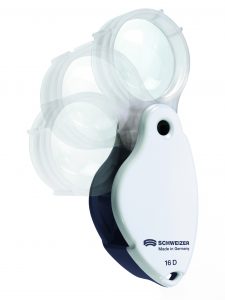
- If the patient has reduced dexterity or a tremor, then a handheld lens may not be ideal. Options in these cases may include a stand magnifier, which they can place against the page, to keep it steady. Again having an LED light-source can improve contrast, which is really beneficial. These can go up to very strong magnification levels but the trade off is always with field of vision, so normally opt for the lens which is strong enough to do the task, but not too strong that it reduces the field.

- There are some hands-free options such as a chest magnifier that hangs around the patient’s neck and gives them some magnification for reading or other close-work. These are slightly limited to lower powered magnifications but can be really good for those with mild visual loss. Spectacle mounted devices can provide another good hands-free option provided the patient is able to hold the text close so that it is kept focussed. Quite often it is a case of trying several different devices to see what is going to be most usable for the patient.

- Counselling the patient as to the use of these devices is really important. Also setting their expectations to a realistic level. I don’t always expect that patients will go off and read a lengthy novel with their magnifier, but what I do want is for them to help make everyday tasks easier – for example reading their mail and short periods of reading their newspaper or magazine.
Lighting
This is a crucial area for a lot of visually impaired patients. Damage caused to the eye by a range of conditions such as glaucoma, AMD, cataract, etc. will reduce the patients contrast and also their ability to adapt from one lighting environment to another.
For reading, I often advise that the patient has their room well lit generally, but then use a supplementary reading lamp, directed onto their print. This tends to be best coming over the shoulder and onto the print, avoiding any glare from the sides.
Any light source that mimics daylight tends to be best, and there is a whole range of products available nowadays including LED lamps and halogen lamps which do this very well. Of course on a clear day using daylight in a similar way is a good option.
Lighting within the kitchen is also important and suggest being able to use contrasting colours to make food preparation easier. A great option is a portable battery operated LED pocket light that can be used wherever and whenever the light is needed most.
Electronic aids
This has been one of the most exciting and progressive areas in low visual care over the past decade. There are a huge range of devices being developed specifically for visually impaired individuals. There are devices to help with reading or accessing print, to devices which help them explore their surroundings. Technologies have been developed to scan around the a room and describe to the patient what objects it is detecting and where they are relevant to the patient, so there is a lot going on in this field.
For the scope of this article and what is useful in everyday practice, I think it is incredibly helpful to talk to patients about the potential benefits of electronic devices, to help them with reading. This might be something simple like suggesting they use an electronic reader such as a Kindle or a tablet so they can simply enlarge print to a size that is manageable for them. This may also offer an alternative means of doing their shopping, for example setting up a shopping list on an online provider, or a means of communication through email with enlarged text. There is a range of software that provides greater access to PCs. There is now a generational shift in patients who are now in their 70’s and 80’s who are familiar with computers etc., so this is no longer an alien concept to them and can be readily accessible.

There are also a wide range of specialised electronic devices designed for people with visual impairment. These range from small handheld devices which can be used to enlarge print when they are out and about to larger devices which are stationed in the house for more detailed reading tasks. Handheld digital magnifiers give a higher and wider magnification range than traditional magnifying glasses.
Transportable video magnifiers offer magnification up to 100x with improved viewing comfort as well as being mobile; ideal if you have limited space or wish to read in different locations. They are perfect for reading post, newspapers, books etc.

Desktop video magnifiers offer the most complete solution in terms of features and reading/writing comfort. They are easy to use as material needed to be magnified is simply placed directly below the screen. Some video magnifiers are also available with speech; they can read documents out loud to users and are particularly useful if eyes become fatigued whilst reading.
Standalone reading machines can read text out loud with the push of a single button to those with severe visual loss or blindness.
It is certainly useful to be able to point the patient in the direction of either a local organisation who have these devices for trial or a company supplying them so they can trial equipment for suitability or get a free in-home demonstration to find out how their needs can be met.
Non-optical devices
It is really beneficial to have an awareness of the type of products which are available for other everyday tasks, such as adapted telephones and kitchen equipment. There is a wide range of products that have been adapted for individuals who struggle with everyday tasks, and again being able to point them in the right direction as to where to source these can be a big help. The RNIB for example have an ‘Everyday Living’ catalogue which is worth having a look at just to appreciate what may be out there for patients.
Social support
The final area I want to mention is that of accessing the correct social support for the patient, particularly if it appears that they are struggling with visual impairment.
Depending on which region of UK you work in there will be different organisations who provide this support. It may be the RNIB, or it might be a local Visual Impairment Society, or a charity such as The War Blind or the Macular Society. Having a knowledge of which organisations operate in your area and how to refer patients to them is really important. Most groups will welcome patients whatever their level of visual impairment, and don’t necessarily require the patient to be registered partially sighted or blind. A lot of these groups can provide home visits to the patient to assess whether any practical elements can be improved to help with the everyday living. A lot of them also run regular social groups, which can be excellent, particularly for some elderly patients who live alone, they can have a meal or catch up with other folk who are in a similar situation, and this can be greatly beneficial.
It is always worth checking if a patient is registered partially sighted or blind, if they fall into the relevant categories, so that they are getting the best support possible.
Summary
I really hope that you have found this article useful, primarily as a reminder of what optometrists can do for patients with visual impairment, and having an awareness of the support and technology available out there. It is often the case that patients will be well served by being referred to a specialist low vision service, but as highlighted there are plenty of straightforward ways in which community optometrists can help these patients.
While we often can’t make their vision better or cure the underlying condition for the patient, I view this as a process of trying to understand the needs of the patient and consider what small measures we can take that makes their everyday life a bit easier and allow them to get the most out of the vision that they do have.
Thank you for reading, and as always I welcome any feedback and comments.
My thanks to Optelec for their support and input with this article. Also to Eschenbach Optik of America for their images of their magnifiers. Please visit their website by clicking the link below.
If you or your company would like to support a featured clinical article on the Optometry-Evolution website, please email me at stanleykeys1@icloud.com. Thank you.

This is very clear cut and knowledgeable article to make referrals and for newly optometrist who start their practice with low vision.