A reasonable part of my current hospital role is involved in carrying out cataract assessment clinics, for those patients referred into the hospital for consideration of cataract surgery. These referrals mainly come from our community optometry colleagues, which I hasten to add are generally of a high standard, and occasionally also from GPs.
I thought it might therefore be useful to share a few of the clinical tips I have built up in my time doing these clinics, to help with your decision making when it comes to referring patients for cataract. Hopefully the following points are helpful:
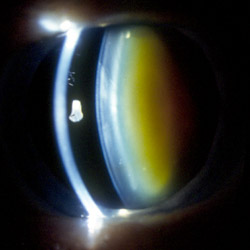 How does the cataract affect the patient?
How does the cataract affect the patient?
This is perhaps the most important factor to consider. To suggest an operation to someone’s eye, they must be experiencing some degree of difficulty relating to the cataract. This might be quite a range of symptoms and problems of varying degrees of severity. Visual acuity alone, we know is not a perfect marker for when cataract surgery needs to be done – glare or poor contrast might for example may be the primary complaint of the patient, while their visual acuity is still 6/9.
The most common reasons I see for patients wanting surgery are probably as follows:
Reading difficulties, reduced distance vision affecting driving and TV, glare when driving, reduced visual function for sports. We always have to be mindful of patients who drive and using this as a guide as to when to suggest surgery on some occasions.
However it is not unknown for a patient not to be listed who might have 6/12 to 6/18 vision, provided they are not driving and are really not complaining of any problems. The old adage of ‘when something is really broken, why try to fix it,’ comes to mind. Some patients on the other hand are driven round the bend by a reduction of vision from 6/5 to 6/6, and almost demand surgery, and may well get listed. One ophthalmology colleague recently put this situation in a good way – ‘ the better the presenting visual acuity, the less likely the patient is to experience improvement with surgery.’ And there is certainly a lot of truth in this.
Consider the type of cataract and how it relates to symptoms
Most cataract types have the potential to reduce visual acuity, however it is useful to consider whether the symptoms tie in with the nature of cataract.
Nuclear – reduce VA and contrast/colours
Cortical – reduce VA, glare, monocular diplopia
Posterior subcapsular – reduced VA, poor reading function.
Is there any other cause for the reduced vision or other symptoms?
I strongly suspect that the vast majority of patients in the UK being referred for surgery have a dilated examination with volk lens prior to being referred, which is great. The main co-morbities as you would expect are conditions such as AMD, glaucoma, previous vein occlusions, amblyopia, macular holes etc. Sometimes of course in the case of dense cataracts, viewing the funds is very difficult, and so we advise the patient from an early stage that the potential outcome of surgery is uncertain as a result, to avoid disappointment. With co-morbidities we try to weigh up as best possible how much of the change is due to cataract, and how much is due to their macular degeneration for example. Previous records of the patient are incredibly useful in these cases. One guide I use, is how clearly i can see the fundus – if it is really clearly viewed through the cataract, then the chance of the removal of this improving visual function in a patient with moderate macular changes is slim. Again giving the patient a guarded prognosis from an early stage is vital.
Any factors which might make surgery higher risk?
Certain changes and features can make the complication risk higher, and these are a few:
Fuchs endothelial dystrophy – post-operative corneal oedema/decompensation
Pseudoexfoliation syndrome – weaker lens zonules, higher risk of dropping the lens. Similarly patients who are over the age of 90 start to get slightly weaker zonules.
High myopia – retinal detachment.
Blepharitis – if this is marked, the risk of endophthalmitis is higher and pre-op lid cleaning measures should be taken.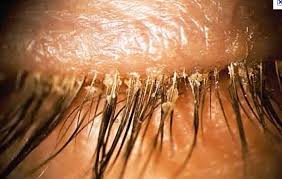
‘Only eye’ patients – the risk of serious complication in a patient’s one good eye becomes a more significant consideration
Patient factors – difficulty in lying flat or still during surgery. Perhaps they may be very anxious.
This is not an exhaustive list by any means, but are some of the main factors to look out for, and really useful to highlight in referral information.
…..and finally – does the patient potentially want an operation?
This is one of the most important factors to suss out. Again this goes back to the nature and level of symptoms they are experiencing, and if it is diminishing their quality of life to some degree. Always good to ask this of the patient before referring. It is worth bearing in mind that the patient may have other significant health treatments ongoing, and the thought of another operation and hospital visits at a certain point in time may not appeal very much.
This was just a very brief look at this whole topic, as there are a lot of factors which come into play, but hopefully this has been a useful post, and as always, comments and feedback are very welcome!
Stan

Just had a discussion in our optometry forum regarding the tendency of some ophthalmologists to operate on minimal cataracts, when patients are asymptomatic. Obviously all cases need to be assessed on their individual merits, but there are certainly some surgeons who are far too gung-ho about operating when vision is still close to normal.
Yes – i agree – I have a ‘if its not broken, don’t fix it approach.’
It is really a great and helpful piece of info. I’m glad that you shared this useful information with us. Please keep us up to date like this. Thanks for sharing.